First Aid for Allergic Reactions: What to Do (2026)
By Dr. Sarah Mitchell, Paramedic & Health Writer • Published 4/28/2026

Last updated: April 2026
First Aid for Allergic Reactions: What to Do (2026)
An allergic reaction can strike within minutes — and when it does, knowing exactly what to do can mean the difference between a frightening close call and a fatality. This guide covers the complete first aid response for mild reactions, moderate reactions, and life-threatening anaphylaxis, based on current Australian and international first aid guidelines.
Table of Contents
- Understanding Allergic Reactions
- Mild vs. Severe: How to Assess the Reaction
- Step-by-Step First Aid for Mild Reactions
- Step-by-Step First Aid for Anaphylaxis
- Mild vs. Severe Allergic Reactions — Comparison
- When to Call Emergency Services
- Common Allergens and Hidden Triggers
- Living with Severe Allergies: Prevention and Preparedness
- First Aid Kit Essentials for Allergic Reactions
- Sources & Methodology
- Frequently Asked Questions
Understanding Allergic Reactions
An allergic reaction is the body's immune system overresponding to a substance — called an allergen — that it has mistakenly identified as harmful. When someone with an allergy is exposed to their trigger, their immune system launches a cascade of chemical responses designed to fight off what it perceives as an invader.
Most allergic reactions are inconvenient and uncomfortable but not dangerous. A smaller proportion — those involving the respiratory or cardiovascular systems — can escalate rapidly to become life-threatening within a matter of minutes.
The challenge with allergic reactions is that they are inherently unpredictable. A person who has previously experienced only mild symptoms from a peanut exposure may develop a severe reaction on a subsequent exposure. There is no reliable way to predict how any single allergic episode will progress. This unpredictability is why every allergic reaction deserves prompt attention and careful monitoring.
Allergic reactions are broadly categorised into three severity levels — mild, moderate, and severe (anaphylaxis) — and each level requires a different first aid response. Knowing which category a person falls into, and being able to recognise when a reaction is escalating, is the single most important skill in allergic reaction first aid.
Every household should have a well-stocked first aid kit that includes allergy response supplies — not just for people with known allergies, but for unexpected reactions in guests, children, or anyone new to an environment.
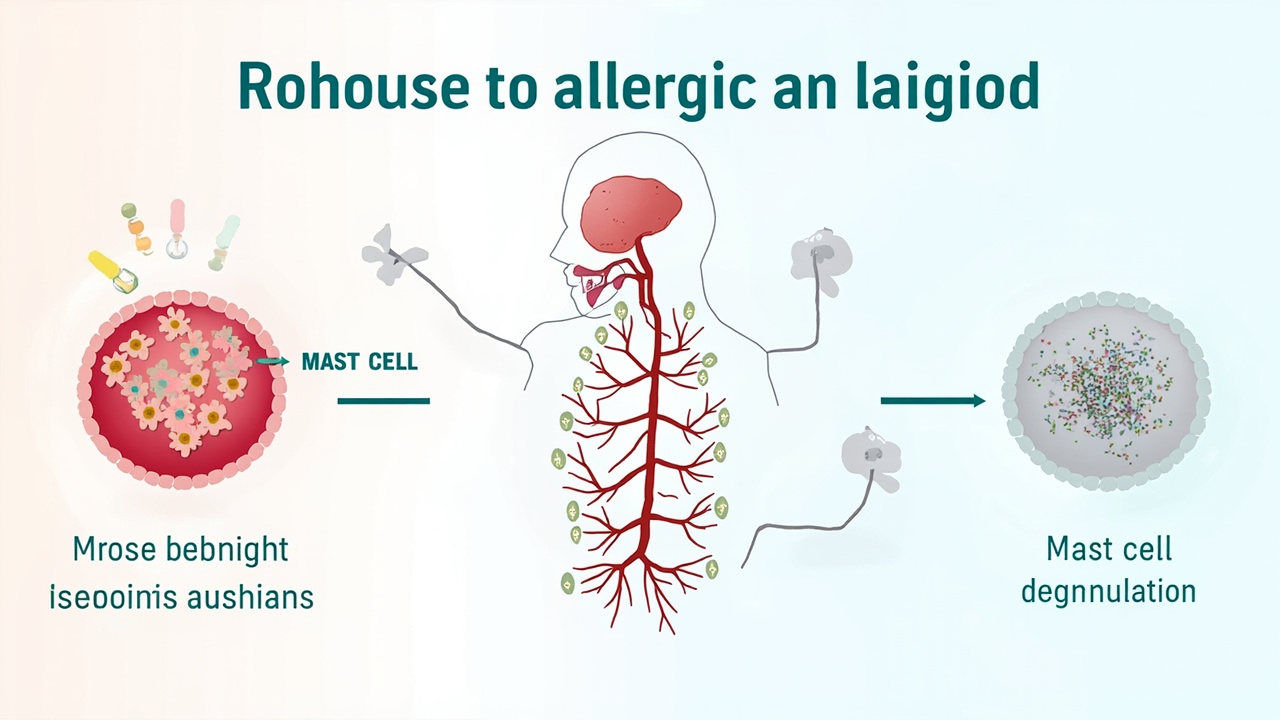
How the Immune System Triggers a Reaction
When an allergen enters the body of a sensitised individual, immunoglobulin E (IgE) antibodies — produced by the immune system in response to a prior exposure — bind to the allergen and trigger mast cells and basophils to release mediators such as histamine, leukotrienes, and prostaglandins. These chemicals cause the symptoms we recognise as an allergic reaction. According to the National Institute of Allergy and Infectious Diseases (NIAID), this IgE-mediated response is the mechanism behind the full spectrum of allergic symptoms, from localised hives to systemic anaphylaxis. Understanding this cascade explains why antihistamines alone cannot stop a severe reaction — they address one mediator but not the broader immune cascade driving anaphylaxis.
Mild vs. Severe: How to Assess the Reaction
Mild Allergic Reactions
Mild reactions typically affect only one body system, most commonly the skin. Symptoms may include:
- A few isolated hives (small, itchy red bumps)
- Mild itching or skin irritation
- A runny nose or mild hay-fever type symptoms
- Minor stomach discomfort
A person experiencing a mild reaction will generally remain alert, able to speak in full sentences, and show no signs of breathing difficulty. Their lips and tongue should appear normal. Their blood pressure will be stable — they will not be dizzy or appear pale and clammy.
Mild reactions, while uncomfortable, are not immediately dangerous. However, they can be a precursor to a more serious reaction, so the person should be monitored closely for any change in condition.
Moderate Allergic Reactions
Moderate reactions indicate that more than one body system is involved, but the life-threatening features of anaphylaxis are not yet present. Symptoms may include:
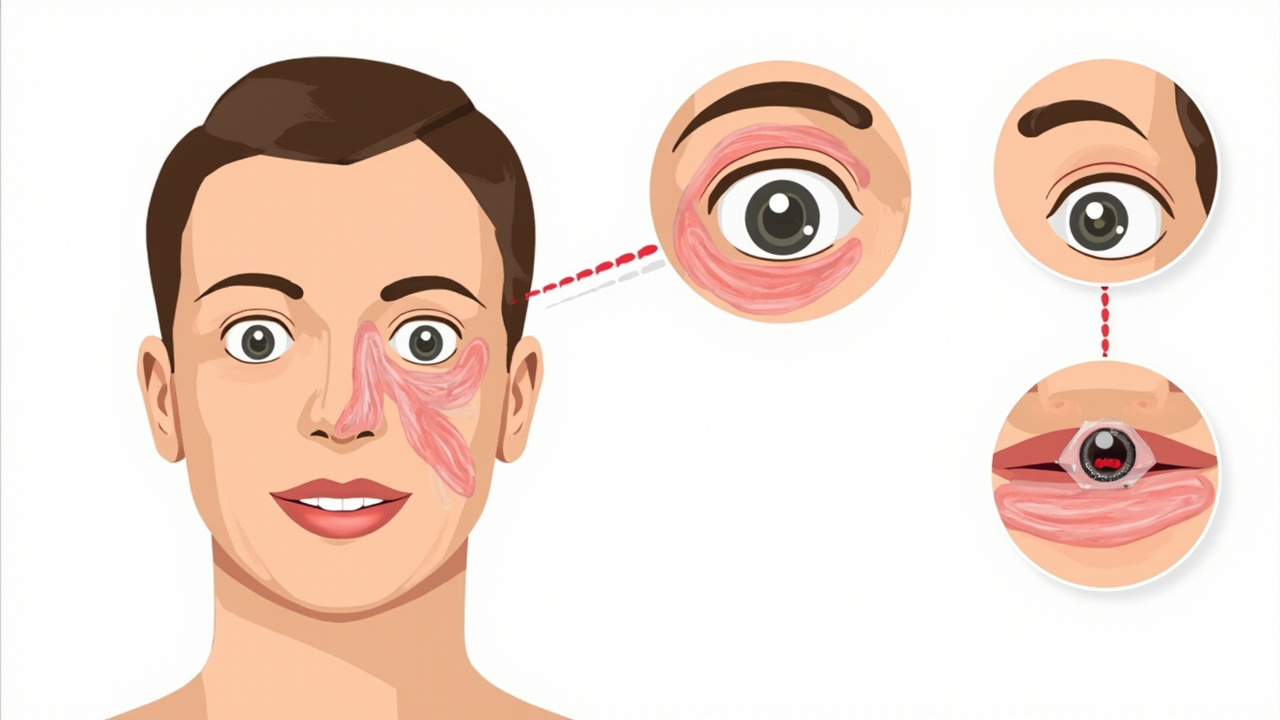
- Swelling of the lips, face, or eyes
- Widespread hives covering larger areas of the body
- Persistent vomiting or abdominal cramping
- Increasing difficulty breathing (mild wheezing)
- Generalised itching and flushing
The critical distinction is that a person with a moderate reaction may still be alert and speaking normally, but the involvement of multiple systems signals that the reaction is escalating. A moderate reaction can progress to anaphylaxis rapidly — sometimes within minutes — particularly if the allergen exposure was significant or if the person has a history of escalating reactions.
Severe Allergic Reactions (Anaphylaxis)
Anaphylaxis is a medical emergency. It is a severe, rapid-onset allergic reaction that affects two or more body systems and can progress to cardiovascular collapse and death within minutes if untreated.
The key warning signs of anaphylaxis include any two or more of the following occurring together after allergen exposure:
- Respiratory symptoms: Difficulty breathing, tightness in the throat, a persistent cough, or audible wheezing
- Cardiovascular symptoms: Sudden dizziness, fainting, pale or clammy skin, weak or rapid pulse
- Skin symptoms: Widespread hives, redness, or significant swelling (beyond one area)
- Gastrointestinal symptoms: Severe vomiting, cramping, or diarrhoea
- Neurological symptoms: Confusion, agitation, or loss of consciousness
A person experiencing anaphylaxis may describe their throat as feeling tight, thick, or like something is stuck. They may be unable to speak, cry, or make sounds. Their skin may appear pale, grey, or bluish. Any one of these signs demands immediate adrenaline administration and an emergency services call.
According to the Australasian Society of Clinical Immunology and Allergy (ASCIA), adrenaline is the first-line treatment for anaphylaxis — there is no substitute, and delaying it in any way increases the risk of a fatal outcome.
In situations where anaphylaxis is suspected alongside potential spinal injury — such as a fall that preceded the reaction — it is critical to understand proper manual handling and spinal safety before moving the person, even in an emergency.
Recognising a Reaction Escalating in Real Time
One of the most important skills in allergic reaction first aid is the ability to recognise deterioration as it happens. A person who was stable and speaking normally five minutes ago may be struggling to breathe now. According to the American Academy of Allergy, Asthma & Immunology (AAAAI), most anaphylaxis episodes reach peak severity within 30 minutes of allergen exposure, making continuous observation essential. Watch for subtle changes: a progressive hoarseness in voice, the appearance of a scratchy throat, increased heart rate visible at the neck, or a sudden request to sit down because standing feels unsafe. These are not minor concerns — they are escalation signals that should trigger immediate action.

Step-by-Step First Aid for Mild Reactions
For a mild allergic reaction — isolated hives, minor itching, a runny nose — the first aid response is straightforward:
-
Remove or isolate the allergen if possible. If the reaction appears to be food-related, stop eating immediately. If it is a contact reaction from a skincare product or plant, wash the affected area with clean water.
-
Give an oral antihistamine if the person is conscious and able to swallow safely. Products containing cetirizine (brands available at Amazon US: tag=theforge05-20, Amazon AU: tag=doublefury-22), loratadine, or diphenhydramine are effective options. Follow the dosage instructions on the product or the guidance of a healthcare provider.
-
Monitor continuously. Even mild reactions can escalate. Stay with the person and watch for any worsening — new symptoms, swelling, breathing changes, or a sudden deterioration in their condition.
-
Keep the person calm and seated in a comfortable position. Physical activity and stress can worsen certain allergic responses.
-
If symptoms worsen at any point, reassess and escalate immediately to the anaphylaxis protocol below.

When to Upgrade from Mild Reaction Protocols
Even a reaction that begins mildly can deteriorate. According to guidance from the Mayo Clinic, the transition from mild to moderate or severe can happen within minutes, particularly with food allergens or insect stings. Be prepared to move to the anaphylaxis protocol — calling 000 and administering adrenaline — if any of the following appear: swelling beyond the face and lips, any breathing change, dizziness or nausea that feels disproportionate to the skin symptoms, or a sudden and unexplained deterioration in a child's condition. When in doubt, treat it as potentially severe: the risk of acting on a false alarm is far lower than the risk of delaying treatment for a genuine anaphylaxis case.

Step-by-Step First Aid for Anaphylaxis
Anaphylaxis is a time-critical emergency. Every second counts. Follow this sequence:
Step 1 — Call Emergency Services Immediately
Do not wait to see if the symptoms improve. Call 000 (Australia) or your local emergency number the moment you identify a potential anaphylaxis case. Put the phone on speaker so your hands are free. Do not hang up — the operator will stay on the line and provide instructions.
Step 2 — Administer Adrenaline
If the person has an adrenaline autoinjector — commonly known by the brand name EpiPen (available at Amazon US: tag=theforge05-20, Amazon AU: tag=doublefury-22) — administer it immediately.
How to use an adrenaline autoinjector:
- Remove the device from its case and cap
- Hold the device firmly against the outer mid-thigh (the injection can be made through thin clothing)
- Push down and hold for the duration specified in the instructions (typically 3-10 seconds)
- After removing the device, massage the injection site for 10 seconds
- Note the time of injection — this is important for the paramedics
If the person has been prescribed an autoinjector and it is not immediately available, ask if anyone nearby has one. Many public venues, schools, and workplaces keep adrenaline autoinjectors in first aid kits. A comprehensive workplace first aid kit should always include at least one adrenaline autoinjector for emergencies.

Step 3 — Position the Person
- If the person is conscious but having trouble breathing, sit them upright in a comfortable position.
- If they are dizzy, faint, or appear to be going into shock, lay them flat immediately.
- If they are vomiting or unconscious, place them in the recovery position (on their side) to keep their airway clear.
- Do not stand them up or allow them to walk — loss of consciousness can happen rapidly.
Step 4 — Administer a Second Adrenaline Dose if Required
If emergency services have not arrived and the person either worsens or fails to improve within 5-10 minutes of the first dose, administer a second adrenaline autoinjector if one is available. This is why carrying two autoinjectors is recommended by ASCIA for people with known severe allergies.
Step 5 — Monitor Until Emergency Services Arrive
Stay with the person. Continue monitoring their breathing and consciousness. Be prepared to perform CPR if they stop breathing or lose consciousness. Familiarising yourself with CPR steps for adults before an emergency strikes is one of the most valuable preparedness measures you can take.

Why Adrenaline Is the Only First-Line Treatment
Many people wonder why antihistamines cannot be used instead of adrenaline during anaphylaxis. The answer lies in mechanism: antihistamines block histamine, one of several inflammatory mediators released during an allergic reaction, but they do not address the broader cardiovascular and respiratory collapse that characterises severe anaphylaxis. According to the National Institutes of Health (NIH), adrenaline works by constricting blood vessels (raising blood pressure), reducing mast cell degranulation (stopping further mediator release), relaxing bronchial smooth muscle (opening the airway), and increasing cardiac output — all critical actions that no other medication can replicate in an emergency setting.
Mild vs. Severe Allergic Reactions — Comparison
Understanding the Severity Spectrum
| Feature | Mild Reaction | Moderate Reaction | Anaphylaxis (Severe) |
|---|---|---|---|
| Body systems affected | One (usually skin) | Two or more | Two or more rapidly |
| Skin symptoms | Few localised hives or itch | Widespread hives, redness | Extensive hives, flushing, pallor |
| Swelling | None or very mild | Lips, face, eyes | Tongue, throat, entire face |
| Breathing | Normal | Mild wheeze or shortness of breath | Significant difficulty, coughing, wheezing |
| Circulation | Normal | Normal | Dizziness, fainting, rapid weak pulse |
| Consciousness | Alert | Alert | May be confused, agitated, or unconscious |
| First aid response | Antihistamine, monitor | Antihistamine, monitor, prepare adrenaline | Adrenaline immediately, call 000, monitor |
| Time to onset after exposure | 30 min – 2 hrs | 10–30 min | 5–30 min (can be rapid) |
| Risk of fatality | Very low | Low if managed promptly | High without adrenaline |
When to Call Emergency Services
Call 000 (or your local emergency number) immediately if:
- The person shows any signs of anaphylaxis — breathing difficulty, throat tightness, fainting, widespread swelling
- Two or more body systems are involved simultaneously
- The person has a known severe allergy and is experiencing symptoms beyond mild
- The person has been prescribed adrenaline and it is not available or has already been used
- The reaction occurred after a known allergen trigger in a person with no prior allergy diagnosis
- The person loses consciousness at any point
Even if adrenaline has been administered and the person appears to recover, always call emergency services. A biphasic reaction — a second wave of symptoms hours after the initial episode — can occur in approximately 20% of anaphylaxis cases, according to research published in the Journal of Allergy and Clinical Immunology. The person must be observed in a medical facility for at least 4-6 hours after apparent recovery.

What to Tell the Emergency Operator
When you call 000, the operator will ask specific questions. According to St John Ambulance Australia protocols, be ready to report: the person's approximate age, any known allergies, what allergen they were exposed to (if known), the time symptoms started, whether adrenaline has been given and what time, whether the person is conscious and breathing, and any other relevant medical history. Keeping emergency information accessible — on a phone note or medical alert card — removes the need to search for information during a crisis when every second matters.
Common Allergens and Hidden Triggers
Understanding where allergens hide is a critical part of prevention — and not just for the person with allergies. Parents, teachers, workplace first aid officers, and anyone responsible for preparing food should understand common allergen risks.
Food Allergens
The most common food allergens causing severe reactions are:
- Peanuts and tree nuts — peanut allergy is among the most common causes of fatal anaphylaxis in children and adults
- Shellfish — prawns, lobster, crab, and other crustaceans
- Eggs — particularly raw or undercooked egg
- Milk — cow's milk allergy is common in young children
- Soy and wheat — more common in children but can persist into adulthood
- Fish — reactions can be triggered by cooking vapours as well as ingestion
Non-Food Allergens
- Bee and wasp stings — venom allergy is a significant cause of anaphylaxis in adults
- Latex — found in rubber gloves, balloons, and some medical devices
- Medications — penicillin and related antibiotics are the most common medication triggers
- Pollens and dust mites — typically cause respiratory allergies, but can trigger severe reactions in susceptible individuals
Hidden Triggers to Watch For
Many people with severe allergies have experienced reactions from trace allergen exposure — a peanut protein invisible to the naked eye on a shared bench, a sauce made with peanut oil not listed on the menu, a child kissed by someone who ate a peanut butter sandwich an hour earlier.
Being allergy-aware is not just about reading labels — it is about understanding cross-contamination risks, communicating clearly in social situations, and never assuming that "a little won't hurt." For someone with a severe allergy, even a trace exposure can be dangerous.

Cross-Contamination Risks in Everyday Settings
Cross-contamination is one of the most misunderstood and underestimated risks for people with food allergies. According to the U.S. Food and Drug Administration (FDA), allergen cross-contact occurs when a residue or trace amount of an allergen is transferred from one food or surface to another — and it can occur at every stage from manufacturing to food preparation at home or in restaurants. A fryer used for chicken wings cooked in buttermilk may contain traces of dairy protein; a knife used to cut a cheese sandwich can transfer milk proteins to bread cut for a allergic child. These invisible exposures are why restaurants in Australia are required by law to be able to answer questions about allergen management in their kitchens, and why many allergy organisations recommend that people with severe allergies avoid fried foods prepared in shared oil.
Living with Severe Allergies: Prevention and Preparedness
For someone with a known severe allergy, the goal is to prevent reactions and be fully prepared when they occur.
Carrying Medication
Anyone with a diagnosed severe allergy should carry their adrenaline autoinjector at all times. This is not optional — it is a fundamental safety requirement. The device should be in a clearly labelled pouch that is immediately accessible, not buried in a bag.
Many countries, including Australia, have laws that allow adrenaline autoinjectors to be carried without a prescription in a first aid kit. Schools, workplaces, and public venues are increasingly stocking them.
Medical Identification
A medical alert bracelet or necklace is one of the most important safety items a person with severe allergies can wear. In an emergency where the person cannot communicate, first responders can look for this identification and understand the cause of the collapse immediately.
Reading Labels and Communicating
People with severe food allergies must develop the habit of reading every label, every time — formulations change without notice. When dining out, communicating the allergy clearly to staff — not just ordering carefully but specifically alerting the manager or chef — can be the difference between a safe meal and a dangerous one.
Regular Check-ups
Allergy testing and review appointments with an immunology specialist should be attended regularly. Allergy profiles can change over time, and new treatments — such as oral immunotherapy for peanut allergy — are becoming increasingly available.
For anyone managing chronic allergy-related conditions, the broader principles of inflammation management and immune system support can be worth exploring alongside conventional treatment. Resources on anti-inflammatory diet and lifestyle approaches at AntiInflammatoryBasics.com offer evidence-based guidance on supporting immune health through nutrition and lifestyle factors, which may complement allergy management under the supervision of a medical practitioner.
Teaching Children About Their Allergies
For children with severe allergies, age-appropriate education is as important as any medication. According to the National Institute of Allergy and Infectious Diseases (NIAID), children as young as three or four can learn to recognise their allergy triggers, avoid sharing food, and tell an adult if they feel a reaction starting. Parents and caregivers should work with schools and childcare providers to develop individualised allergy action plans, ensure adrenaline autoinjectors are accessible and not locked away, and train staff in recognising symptoms. An anaphylaxis action plan completed with a child's immunology specialist — typically using the ASCIA Action Plan format — gives school staff clear, written guidance on exactly what to do if a reaction occurs.
First Aid Kit Essentials for Allergic Reactions
Every home and workplace first aid kit should contain items for managing allergic reactions. The contents should be checked regularly for expiry dates.
Essential Items
| Item | Purpose | Notes |
|---|---|---|
| Adrenaline autoinjector (EpiPen Jr or Adult) | First-line treatment for anaphylaxis | Requires prescription; expiry date must be checked monthly |
| Oral antihistamine (cetirizine or loratadine) | Treatment for mild-moderate reactions | Liquid format for children; follow dosing guides carefully |
| Corticosteroid tablet (e.g. prednisolone) | Secondary treatment for severe reactions | Some plans include this for extended reactions; requires prescription |
| Disposable gloves | Protection when assisting another person | Essential for hygiene during any first aid response |
| Saline wash or eye rinse | Flushing allergens from eyes after contact reactions | Sterile saline in single-use ampoules |
| Cotton triangular bandage | Securing cold compresses, arm slings | Versatile first aid item |
| Instant cold compress | Reducing swelling from localised reactions | Activate by squeezing — no refrigeration needed |
| Medical alert identification (bracelet or card) | Communicating allergy status in an emergency | Essential for anyone with diagnosed severe allergy |
| First aid reference card | Step-by-step anaphylaxis response protocol | Laminate and keep in kit for quick reference |
A comprehensive first aid kit for households or workplaces that include members with severe allergies should include at least two adrenaline autoinjectors, as some severe reactions require a second dose before emergency services can arrive. If you are assembling or upgrading your kit, review our complete guide to first aid kit contents to ensure nothing essential is missing.

Checking and Maintaining Your Kit
An expired adrenaline autoinjector is useless in an emergency. According to the Australasian Society of Clinical Immunology and Allergy (ASCIA), adrenaline degrades over time even when stored correctly, meaning an expired device cannot be relied upon to deliver the correct dose. Schedule a monthly check: verify the expiry date on the autoinjector label, confirm the liquid inside is clear (not brown or cloudy), and ensure the safety cap is intact. Replace any expired devices immediately. Keep a spare in your kit even if you carry one on your person — having two available is the standard of care recommendation for people at risk of severe reactions.

Sources & Methodology
Guideline Alignment and Evidence Review
-
Australasian Society of Clinical Immunology and Allergy (ASCIA) — Anaphylaxis Guidelines: ASCIA is the peak professional body for clinical immunology and allergy in Australia and New Zealand. Their anaphylaxis action plans and guidelines form the foundation of Australian first aid response protocols for severe allergic reactions. Available at: https://www.allergy.org.au
-
American Academy of Allergy, Asthma & Immunology (AAAAI) — Anaphylaxis Overview: Comprehensive clinical overview of anaphylaxis including pathophysiology, triggers, and emergency management. Available at: https://www.aaaai.org
-
Mayo Clinic — Allergic Reactions and Anaphylaxis: Detailed guide to recognising and responding to allergic reactions, including when to seek emergency care. Reviewed by clinical staff. Available at: https://www.mayoclinic.org/diseases-conditions/anaphylaxis
-
National Institute of Allergy and Infectious Diseases (NIAID) — Food Allergy Guidelines: The NIAID, part of the U.S. National Institutes of Health, coordinates federal allergy research and publishes clinical guidelines on food allergy management, anaphylaxis prevention, and allergen immunotherapy. Available at: https://www.niaid.nih.gov
-
National Institutes of Health (NIH) — MedlinePlus Anaphylaxis Resource: Peer-reviewed consumer health information on anaphylaxis mechanism, triggers, and emergency treatment, maintained by the U.S. National Library of Medicine. Available at: https://medlineplus.gov/anaphylaxis.html
-
U.S. Food and Drug Administration (FDA) — Food Allergen Labeling Guidance: Regulatory guidance on major food allergens, cross-contamination risks, and allergen labelling requirements for consumers and industry. Available at: https://www.fda.gov/food/food-allergensgluten-free-guidance-documents-regulatory-information/food-allergen-labeling-requirements
-
Journal of Allergy and Clinical Immunology — Biphasic Anaphylaxis Research: Peer-reviewed research on the incidence and management of biphasic allergic reactions, indicating approximately 20% of anaphylaxis cases involve a second wave of symptoms. Available at: https://www.jacionline.org
-
Australian Red Cross — First Aid for Allergic Reactions: Evidence-based first aid guidance aligned with Australian and international standards, including anaphylaxis response protocols. Available at: https://www.redcross.org.au/first-aid
-
St John Ambulance Australia — Anaphylaxis Emergency Response: Step-by-step emergency protocols for first responders managing anaphylaxis, including adrenaline administration guidance. Available at: https://www.stjohn.org.au
-
World Allergy Organization (WAO) — Anaphylaxis Guidelines: International clinical guidelines on the diagnosis and management of anaphylaxis across all age groups. Available at: https://www.worldallergy.org
Frequently Asked Questions
Common Questions About Allergic Reactions
What is the first thing you should do when someone has an allergic reaction?
The first step is to assess the severity of the reaction. For mild symptoms like a few hives or minor itching, monitor the person closely and consider giving an antihistamine. For moderate symptoms such as swelling of the lips or face, or any hint of breathing difficulty, call emergency services immediately and administer an adrenaline autoinjector if one is available.
How do I use an adrenaline autoinjector (EpiPen)?
Remove the autoinjector from its case and remove the safety cap. Firmly push the tip against the outer thigh — you can inject through clothing. Hold it in place for 3-10 seconds (following the specific product instructions). Massage the injection site for 10 seconds afterward. Call emergency services immediately after the injection, even if the person appears to recover.
What is anaphylaxis and how do I recognise it?
Anaphylaxis is a severe, potentially fatal allergic reaction that affects multiple body systems at once. Warning signs include: difficulty breathing or wheezing, swelling of the tongue or throat, a widespread rash or hives, a sudden drop in blood pressure causing dizziness or fainting, and gastrointestinal symptoms like severe vomiting or cramping. Two or more of these symptoms occurring together after an allergen exposure is a strong indicator of anaphylaxis.
Should I give someone antihistamines during a severe allergic reaction?
Antihistamines are not effective during anaphylaxis because they work too slowly — the reaction is already overwhelming the body by the time symptoms appear. Adrenaline is the only first-line treatment for anaphylaxis. Antihistamines may be given AFTER emergency services have been called and AFTER adrenaline has been administered, as a secondary measure to manage lingering symptoms.
Can someone die from an allergic reaction without immediate help?
Yes — anaphylaxis can be fatal within minutes if untreated. Fatal anaphylaxis most commonly occurs when adrenaline is not administered in time, when the person is alone and unable to call for help, or when the reaction begins with a sudden airway blockage before any other symptoms are apparent. This is why calling emergency services immediately is as critical as administering adrenaline.
What is a biphasic allergic reaction?
A biphasic reaction is a second wave of allergic symptoms that occurs hours after the initial reaction appears to have resolved. Research published in the Journal of Allergy and Clinical Immunology suggests biphasic reactions occur in approximately 20% of anaphylaxis cases. This is why anyone who experiences anaphylaxis should be monitored in a emergency department for at least 4-6 hours, even after they appear to have recovered.
How should I store an adrenaline autoinjector at home?
Adrenaline autoinjectors should be stored at room temperature — between 15°C and 25°C — and protected from direct sunlight and extreme cold. Do not refrigerate them. Check the expiry date regularly and replace expired devices immediately. Keep autoinjectors in a clearly labelled, easily accessible location that all household members know, and ensure everyone in the household knows how to use it.
Dr. Sarah Mitchell is a practising paramedic and health writer with over 15 years of field experience in emergency pre-hospital care. She holds a Graduate Diploma in Paramedicine from Queensland University of Technology and has spent a significant portion of her career delivering first aid training and writing health education content for general audiences. She is passionate about making evidence-based first aid knowledge accessible to everyone — not just healthcare professionals.